EI Global Symposium 2026
World first event in Zurich was a huge success!
Day 1 of the 2026 EI Global Symposium held at the Careum Auditorium in Zurich, Switzerland. The group comprised 70 delegates from across the world.
To learn more about this special event, please read on…
The main objectives for the EI Global Symposium were to raise awareness of the challenges faced by parents and affected individuals, share knowledge from clinical experts, highlight gaps in our disease understanding, showcase current research, and encourage future research by bringing everyone in our network together.
The event was divided over two days
Day 1) A scientific study day comprised of four sessions including patient and parent experiences, clinical classifications and care, new directions for EI, and gene therapy and gene editing for EI;
Day 2) A day of steering committee meetings designed to generate new research projects, and to develop care guidelines for neonates and infants, care guidelines for children, adolescents and adults, and further care guidelines for the recognition and management of infections.
Day 1 - The Scientific Study Day
This was an incredible day that brought together 70 people from all over the world to share their knowledge, learn from each other, build new connections, and highlight new targets for the future.
Our international group included: 26 EI communtity representatives, 5 nurses, 23 dermatologists, 11 researcher/scientists, and 5 PhD candidates.
Day 1 sessions were just superb, with brilliant and informative talks from 20 guest speakers including patient and parent representatives, educational and psychological specialists, clinical dermatologists, pathophysiology and microbiology scientists, and gene-editing researchers. Many of the speakers were members of our EI Cure Research Alliance and EI Cure Project Grant Awardees sharing progress of their research, and offering hope for the future.
Day 1 was divided into four sessions with the following focus: 1) Patient and Parent Experiences, 2) Clinical Classifications and Care, 3) New Directions for EI, and 4) Gene Therapy and Gene-Editing for EI.
Session 1) Patient and Parent Experiences
The host for the event, Helen Lill welcomed all the speakers and delegates, and thanked everyone for making history by so eagerly attending the very first event dedicated to the care and wellbeing of all those affected with Epidermolytic Ichthyosis.
Helen (Switzerland) presented the first talk for session 1, sharing the results of two surveys conducted within the online EI Support Group. The first was a community survey, with the objective of documenting care routines, symptom burden, and research priorities from the perspective of the EI community. Helen highlighted the top three EI symptoms identified by our community as the greatest priority for research: 1) Blistering, 2) Pain (from cracks, fissures, and blisters), and 3) Infections. The second half of Helen’s talk focused on patient narratives about healthcare barriers and common disease misconceptions that the EI community would like to highlight for the healthcare community.
The second and third talks were focused on daily care routines presented by Catherine Lancashire and Kelly Hough-Coles (United Kingdom), both parents of children affected by KRT 10 EI, and KRT1 EI with Palmoplantar Keratoderma (PPK). Both Cat and Kelly took care to describe all aspects of care that healthcare professionals might not be aware of, such as daily challenges at school, and all the time and energy that goes into trying to educate their communities in order to increase awareness, and reduce social stigma. Cat explained their difficult adjustment to new life as first-time parents, and Kelly demonstrated the level of commitment needed to care for PPK.
The fourth talk in Session 1 was delivered by another parent representative and EI Cure Project Ambassador, Asta Schantz-Conlon (Denmark). Asta shared her experiences of recurrent Group A Streptococcal infection over an 8 month period with her young daughter who is affected with KRT10 EI. Asta shared a common phenomenon for the EI community whereby healthcare practitioners fail to change management despite repeated episodes of infection recurrence. Her talk highlighted the importance of healthcare practitioners working with patients to achieve mutually agreeable outcomes, and the need to seek further advice from experts in infection to help manage recurrences.
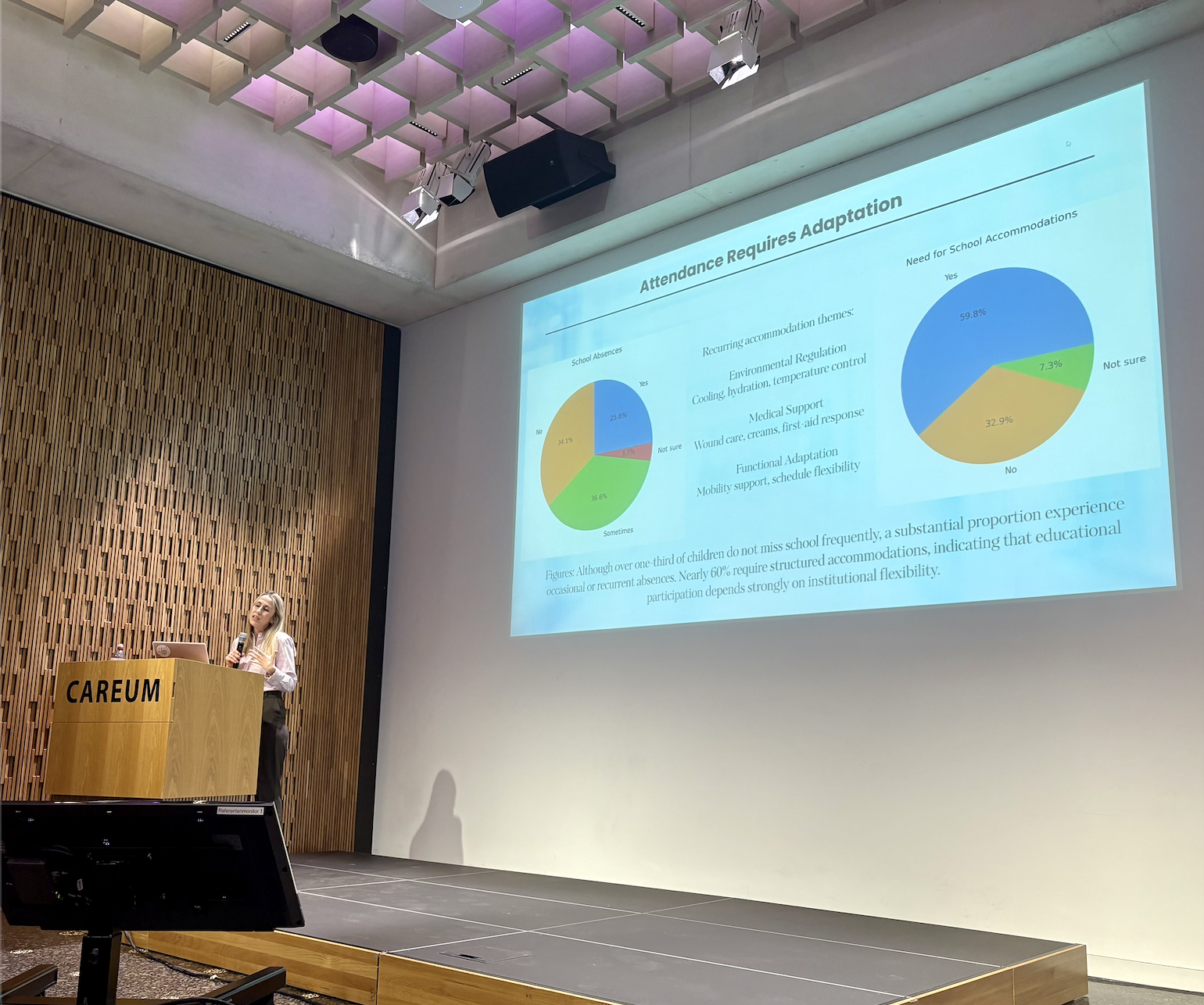
The fifth talk was given by Zoi Argyri (Greece), who learned about EI when she became a teacher to Helen Lill’s youngest daughter, who is affected with KRT10 EI. Zoi decided to dedicate her Masters thesis to better understand the educational and social needs of children with EI from around the world from the perspectives of their caregivers and their teachers. The key messages from Zoi’s presentation conclude that self-image is shaped by the family narrative, and that schools need to consider: the invisible daily burden associated with severe skin diseases; that educational success depends on consistent practical accommodations; and that exclusion at school is often subtle rather than explicit, and needs to be managed appropriately in order to preserve a positive self-image. Zoi’s final note “When inclusion is predictable, resilience becomes visible” resonated with every parent in the room.
The final talk for Session 1 came from Rotem Zvigi (Israel), a parent to a young daughter with KRT10 EI, and a rehabilitation psychologist by profession. Rotem delivered an emotional and very enlightening talk on the psychological impact of severe skin disorders on the sense of self. He made reference to concepts such as having a “Second skin”, and the potential manifestation of a “False self” in response to trauma, and how to help to build a flexible and resilient skin ego together, referred to as the “Coping axis”. He sited the importance of organisations like EI Cure Project to help build community to ensure the sense of self can develop under nurturing and relatable circumstances.
Session 2) Clinical Classifications and Care
Session 2 was designed to explore current best practice, and provide guidance on the care of EI during all stages in life.
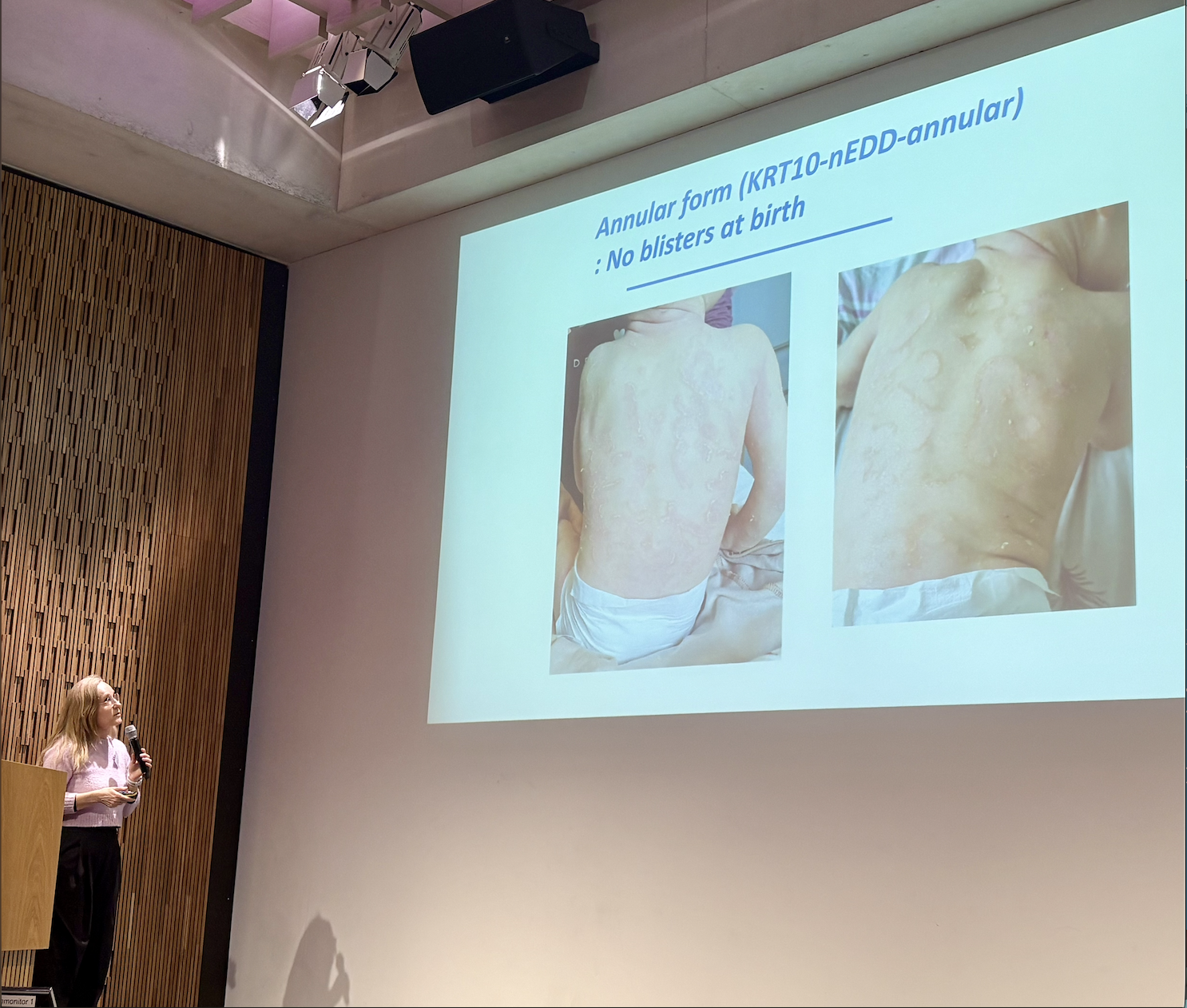
The session started with Professor Juliette Mazereeuw-Hautier (France) in lieu of Dr Angela Hernandez-Martin (Spain) who gave an introduction to the new clinical classification for EI, now clinically referred to as a Non-Syndromic Epidermal Differentiation Disorder (nEDD-Epidermolytic). Professor Mazereeuw explained where the symptoms of EI come from in relation to the histopathology of the skin, in addition to evidence for and against the existence of phenotype-genotype correlations.
The second talk, by Professor Smail Hadj Rabia (France) focused on differential diagnoses at birth and EI care in neonates, followed by Professor Juliette Mazereeuw-Hautier who explored the natural history of EI, including how different phenotypes might change over time.
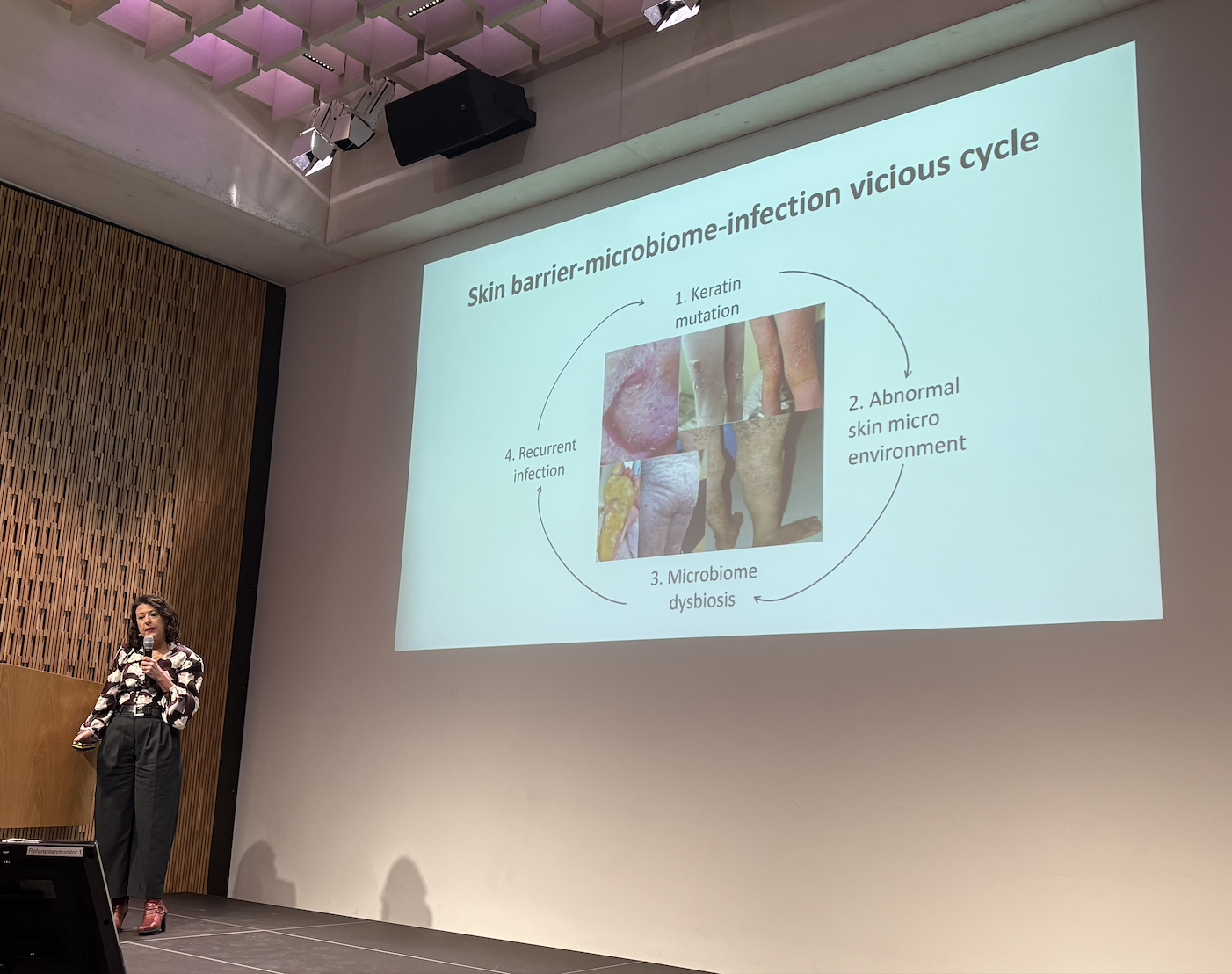
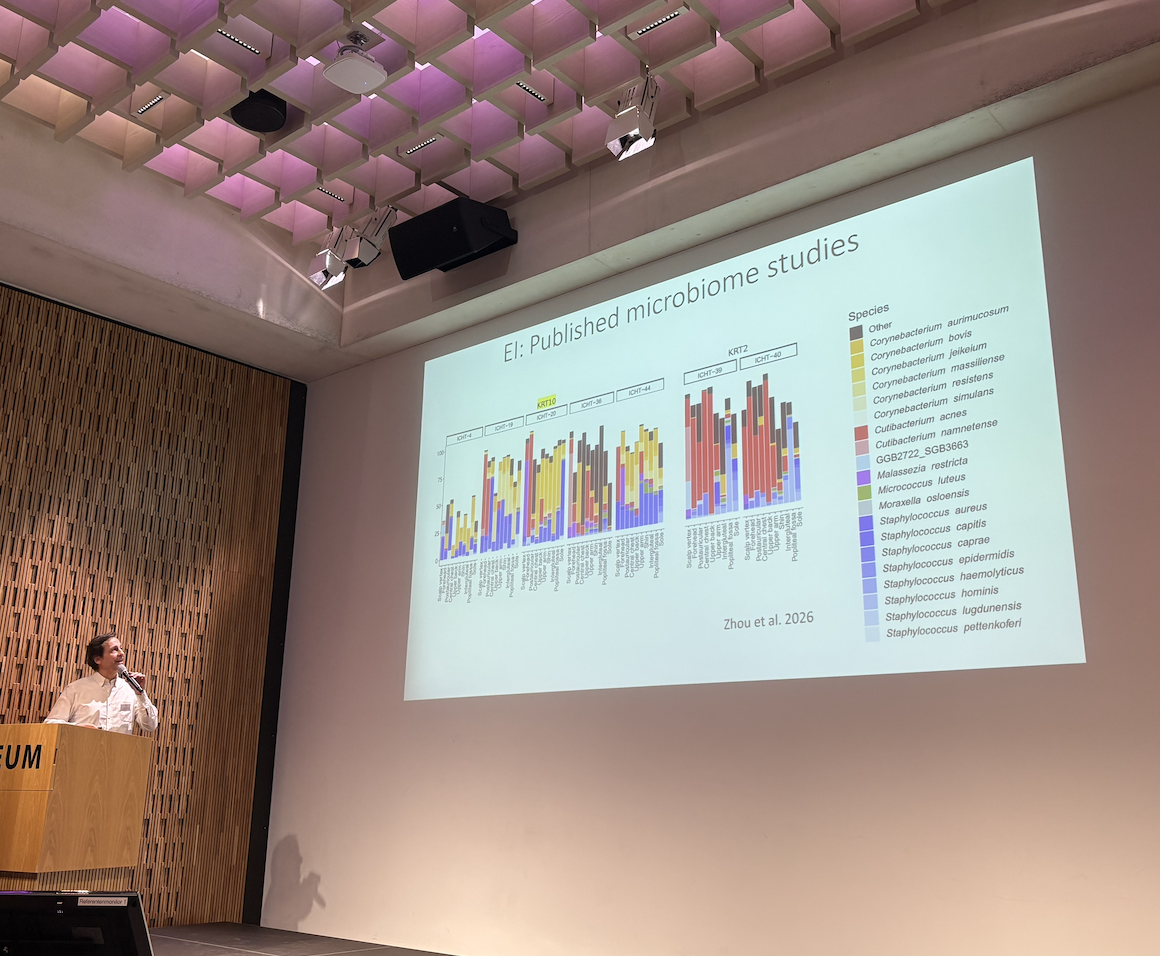
Professor Jemma Mellerio (United Kingdom) gave a very practical and comprehensive talk on how to care for EI skin during adolescence and adulthood, and was followed by two further UK experts, Professor Edel O’Toole and Dr Anna Martinez who shared resources and existing knowledge on how to manage infections in EI, in addition to clinical data on the bacterial and fungal infections seen according to genotype in their London patient population.
Session 3) New Directions for EI
After lunch, the focus of Session 3 shifted away from the realities of living with and managing the symptoms of EI, and moved towards gaining a deeper understanding of the biological mechanisms and pathogenesis behind EI, in order to find new targets for therapeutic intervention.
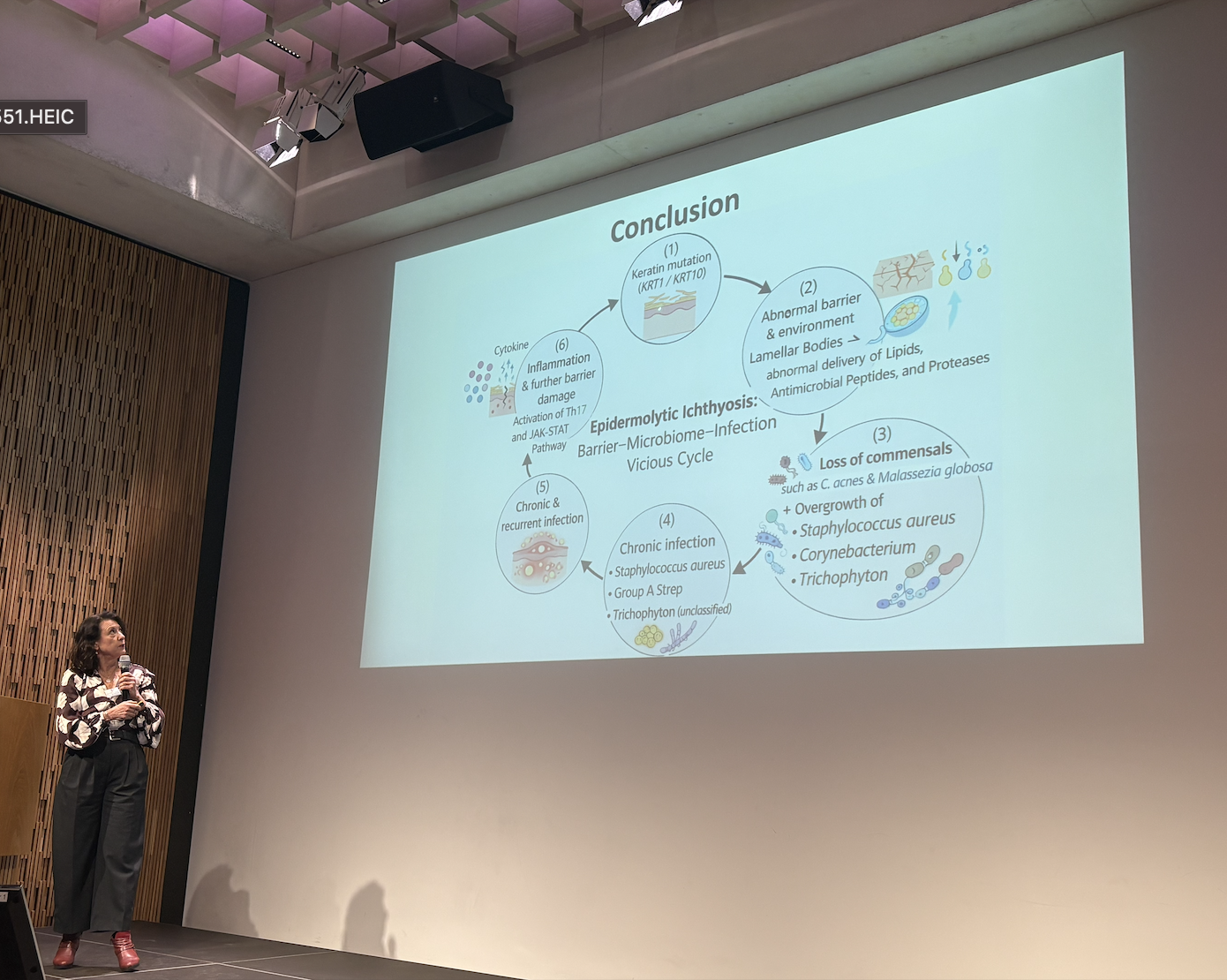
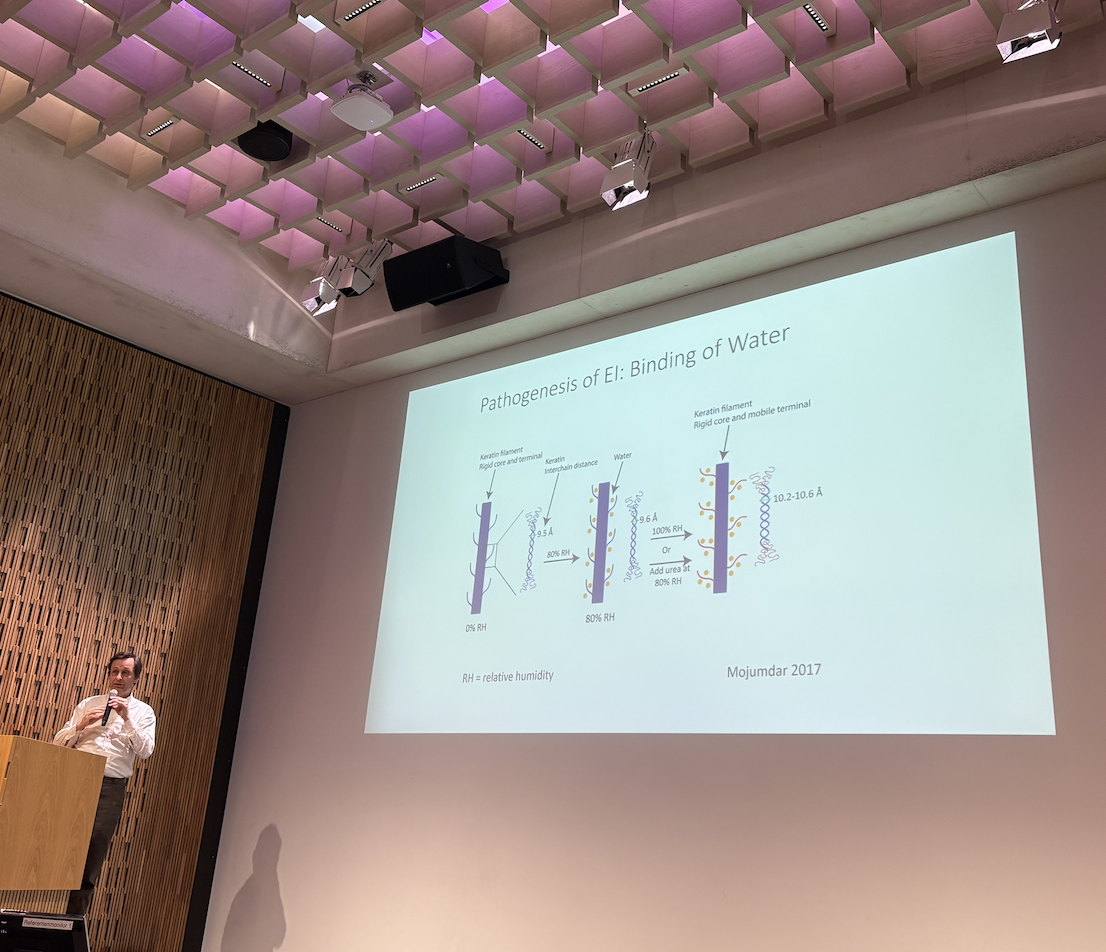
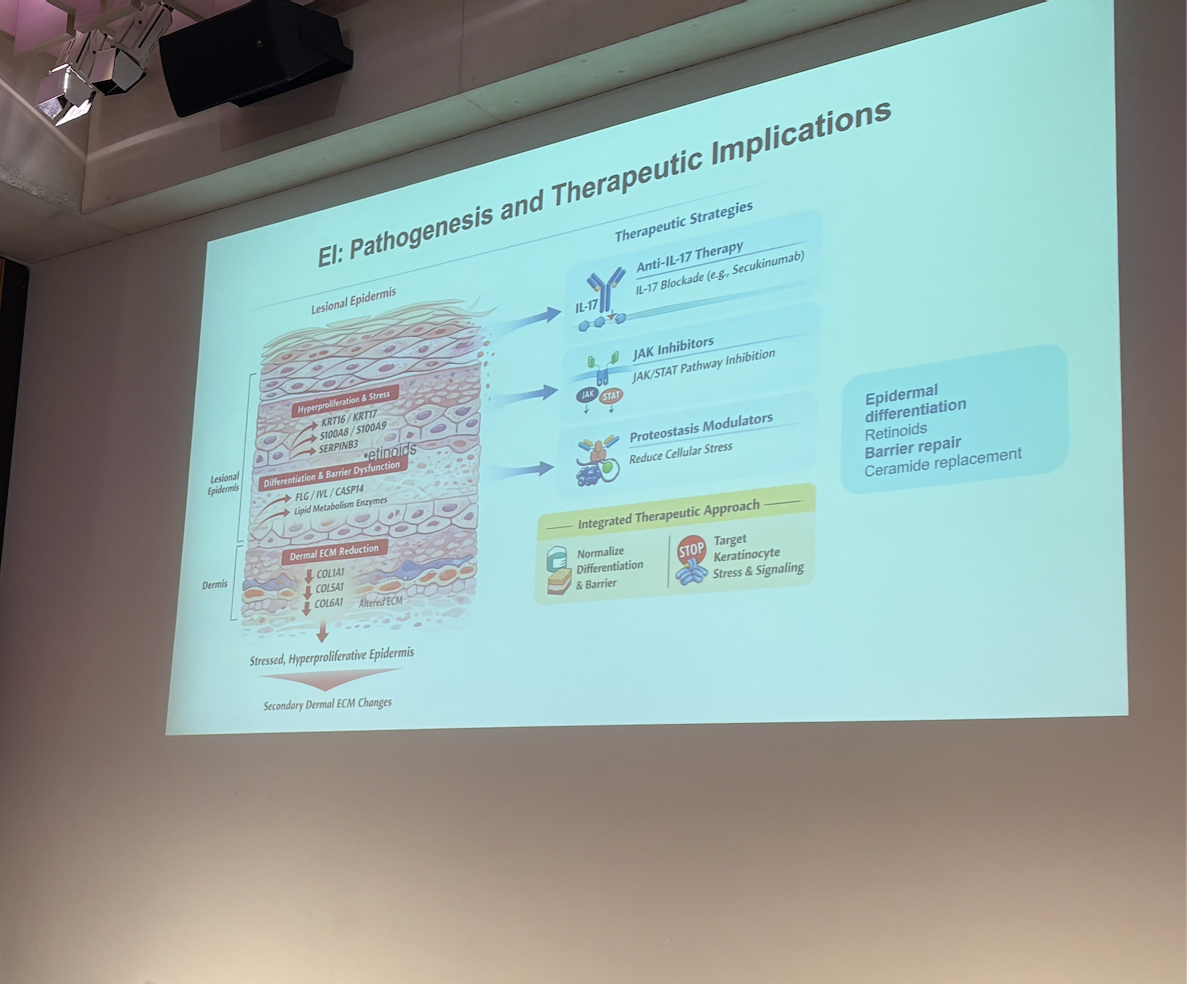
Professor Matthias Schmüth (Austria) gave a detailed talk about the pathogenesis of EI, helping the audience to see many potential therapeutic targets and areas for further exploration on the basis of the basic mechanisms involved in EI biology. Professor Schmüth also made reference to a published case study to demonstrate how quickly EI skin can heal in the right circumstances; an important reference point when considering therapeutic approaches and outcome measures.
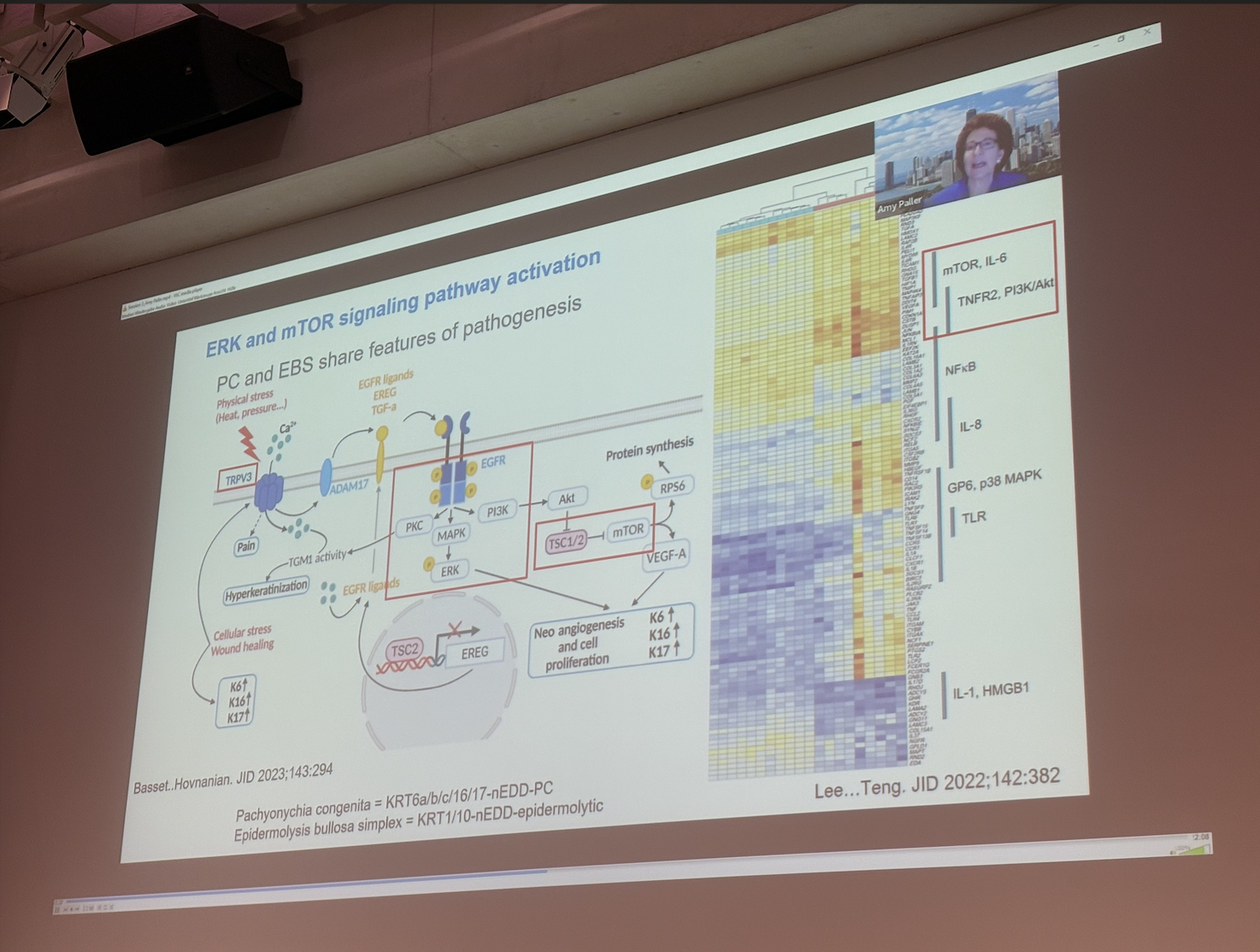
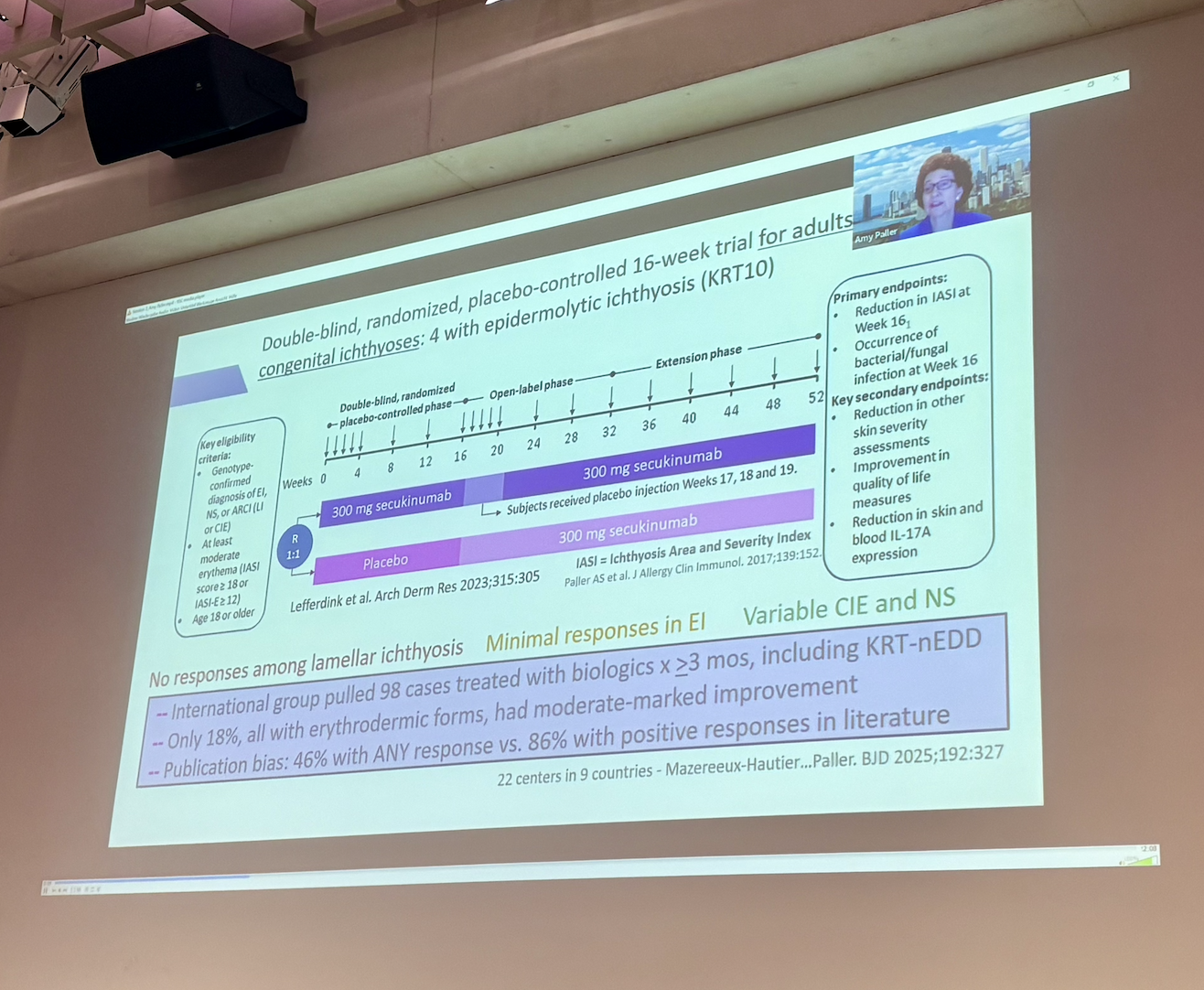
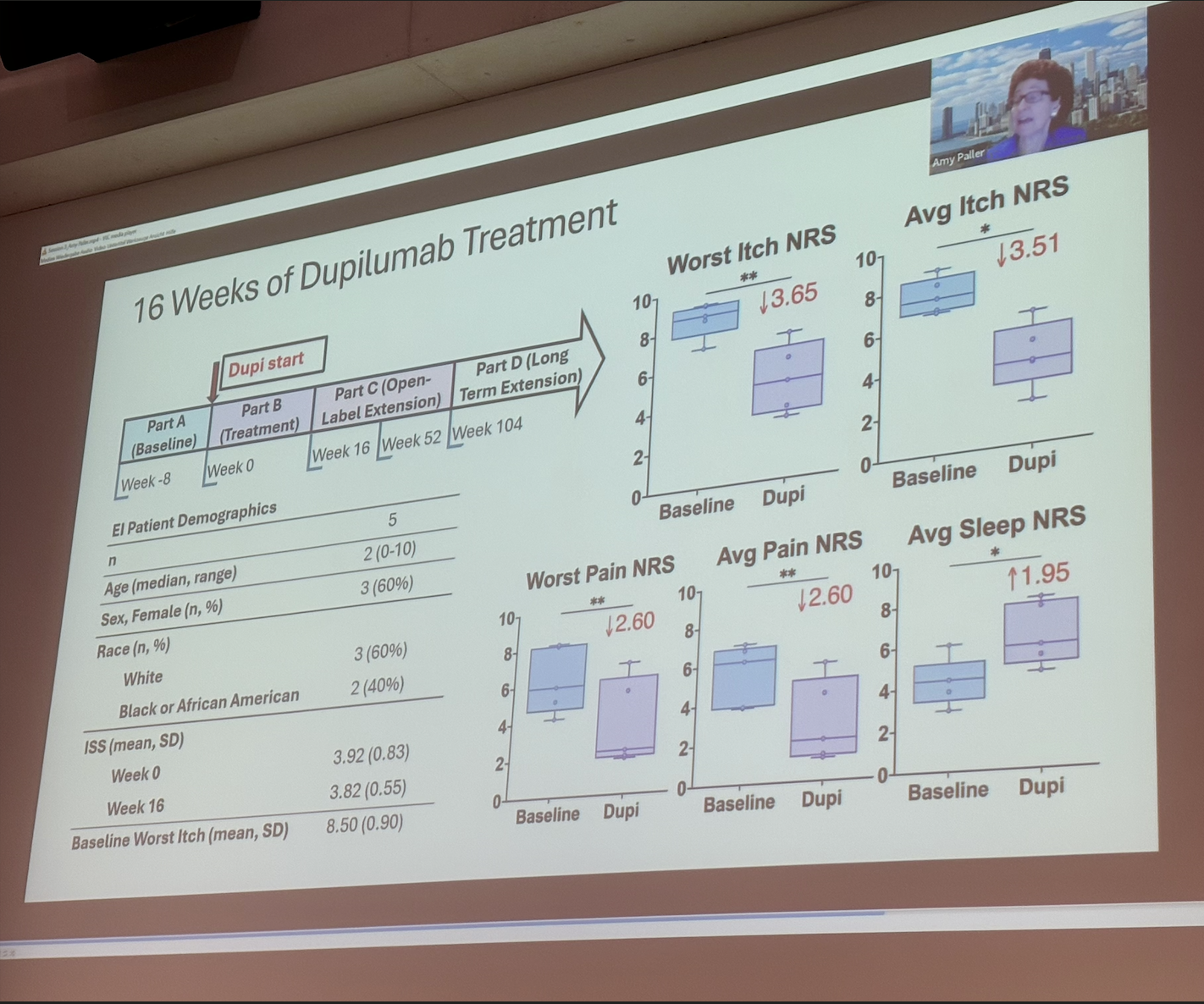
Dr Amy Paller (United States) followed with an extensive talk on the inflammatory pathways observed for EI as potential therapeutic targets. Dr Paller shared data from small EI cohorts involved in broader ichthyosis clinical studies to test the effectiveness of biologics which target the IL-17 pathway. For EI, Dr Paller concluded that the IL-17 pathway has not proved an effective target, and secukinumab and ustekinumab were not found to improve standard ichthyosis outcomes after 16 weeks of treatment compared with a placebo. Dr Paller did show some data to indicate that Dupilimab may be helpful in the treatment of excessive itch for EI patients, however there was no other evidence of skin symptoms improving with Dupilimab, only itch scores improved. Following this revelation, Helen Lill opened some discussion with the audience to ask for a show of hands from those with experience of using Dupilimab. A number of clinicians reported similar findings of improved itch, but no major improvements in disease severity overall. Dr Paller also suggested that Erlotinib may hold some promise for EI (specifically KRT1 with PPK) on the basis that positive results have already been reported with another Keratinisation disease, Pachyonychia Congenita where patients with PPK report improvements in pain and reduced hyperkeratosis.
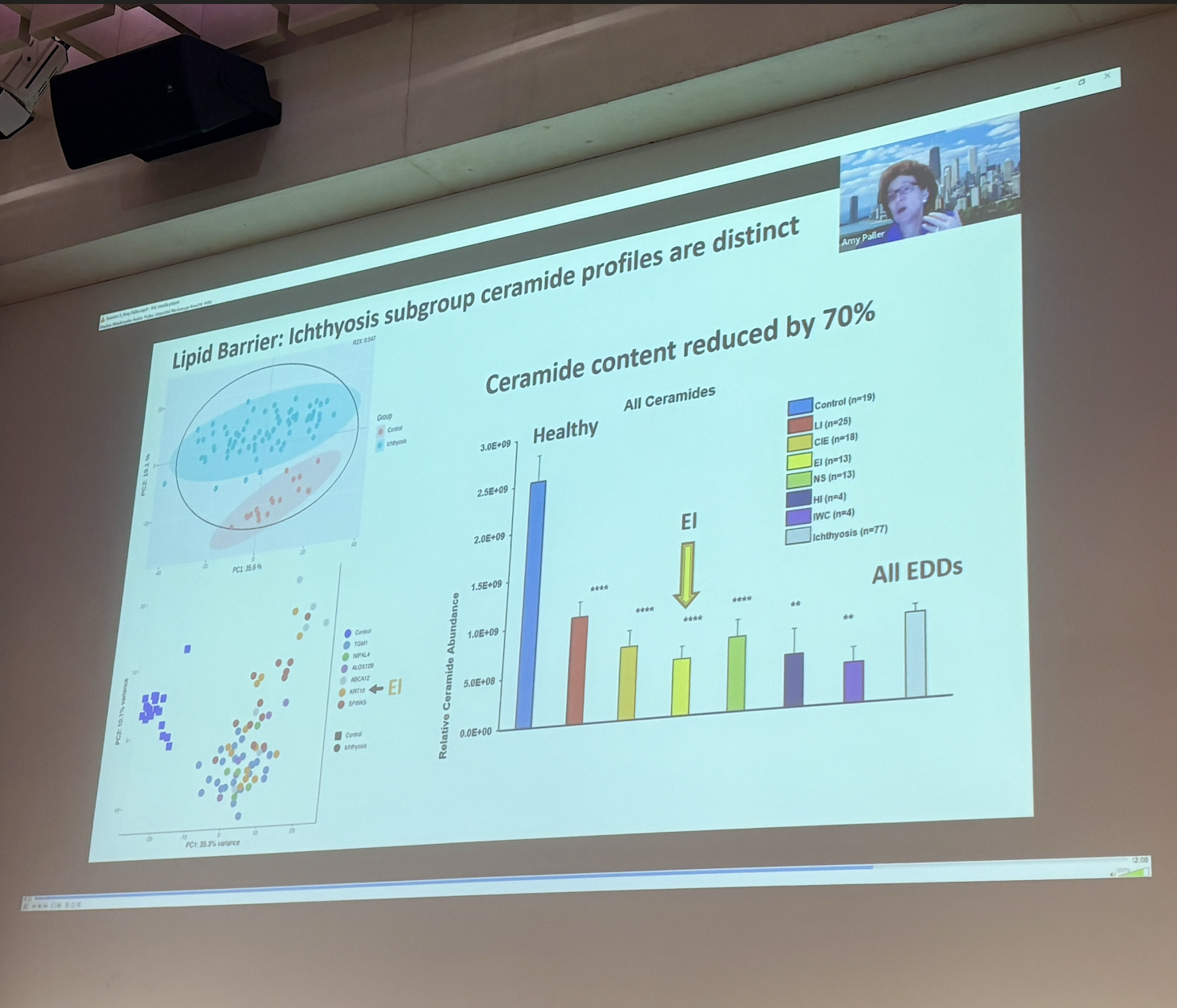
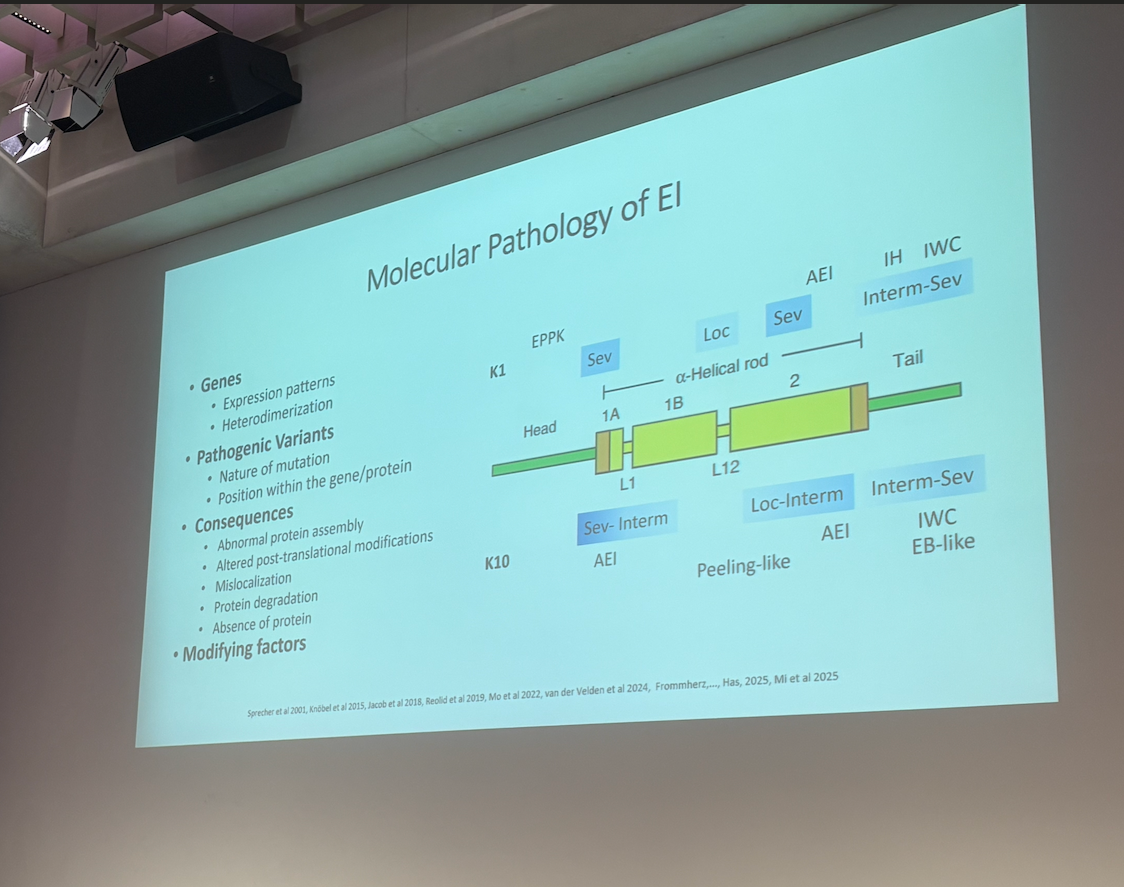
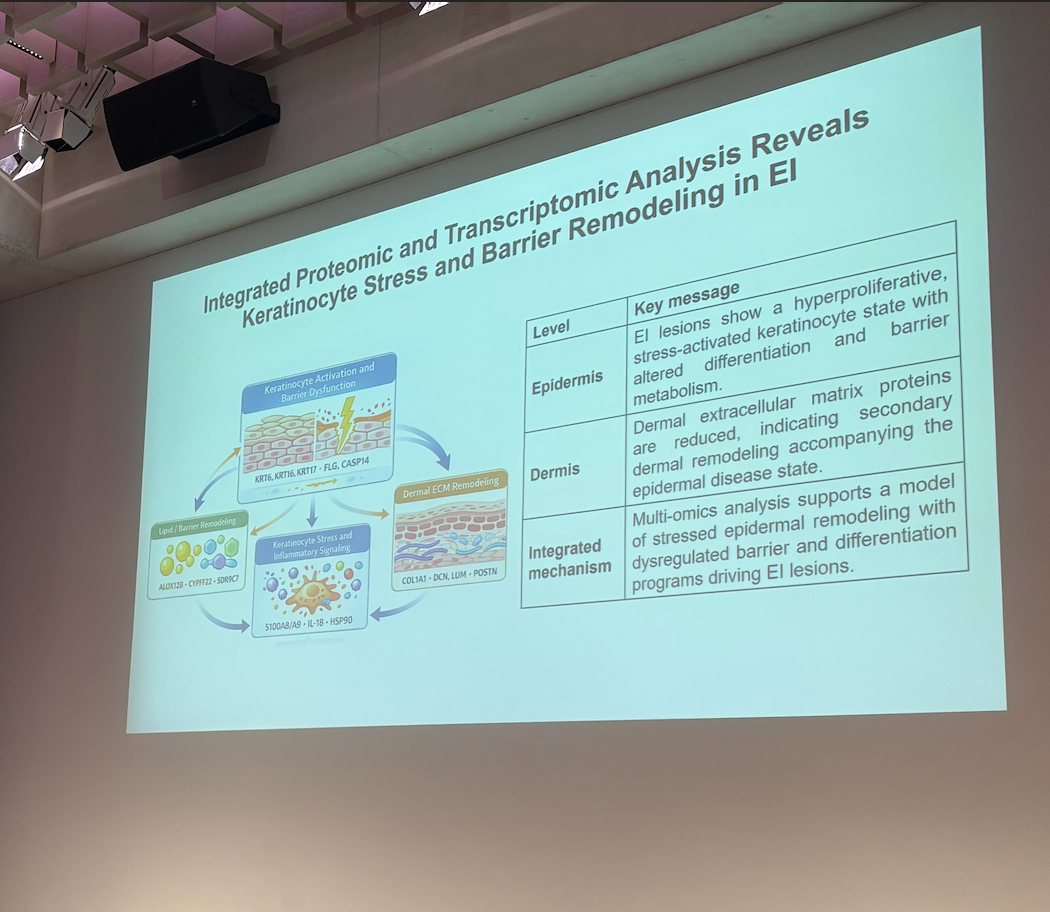
Professor Cristina Has (Germany) shared new data from a recent EI Cure Project funded study to explore proteomic and RNA-sequencing data for EI. Professor Has was able to explain some correlations in genotype (including IWC, AEI, K1, K10) and phenotype (disease severity) in accordance with molecular pathology and the position of the mutation within the helical rod of the gene. Professor Has was able to describe in detail the drivers behind the impaired skin barrier, hyperkeratosis, and keratinocyte stress seen in EI as part of the IL-18 inflammatory pathway, revealing a potential new therapeutic target. Professor Has concluded that an integrated therapeutic approach may be needed in order to normalise cell differentiation and the skin barrier in addition to reducing keratinocyte stress; this could include a combination of approaches including IL-17/1L-18 blockade, JAK inhibition, and Protease modulation to reduce cellular stress.
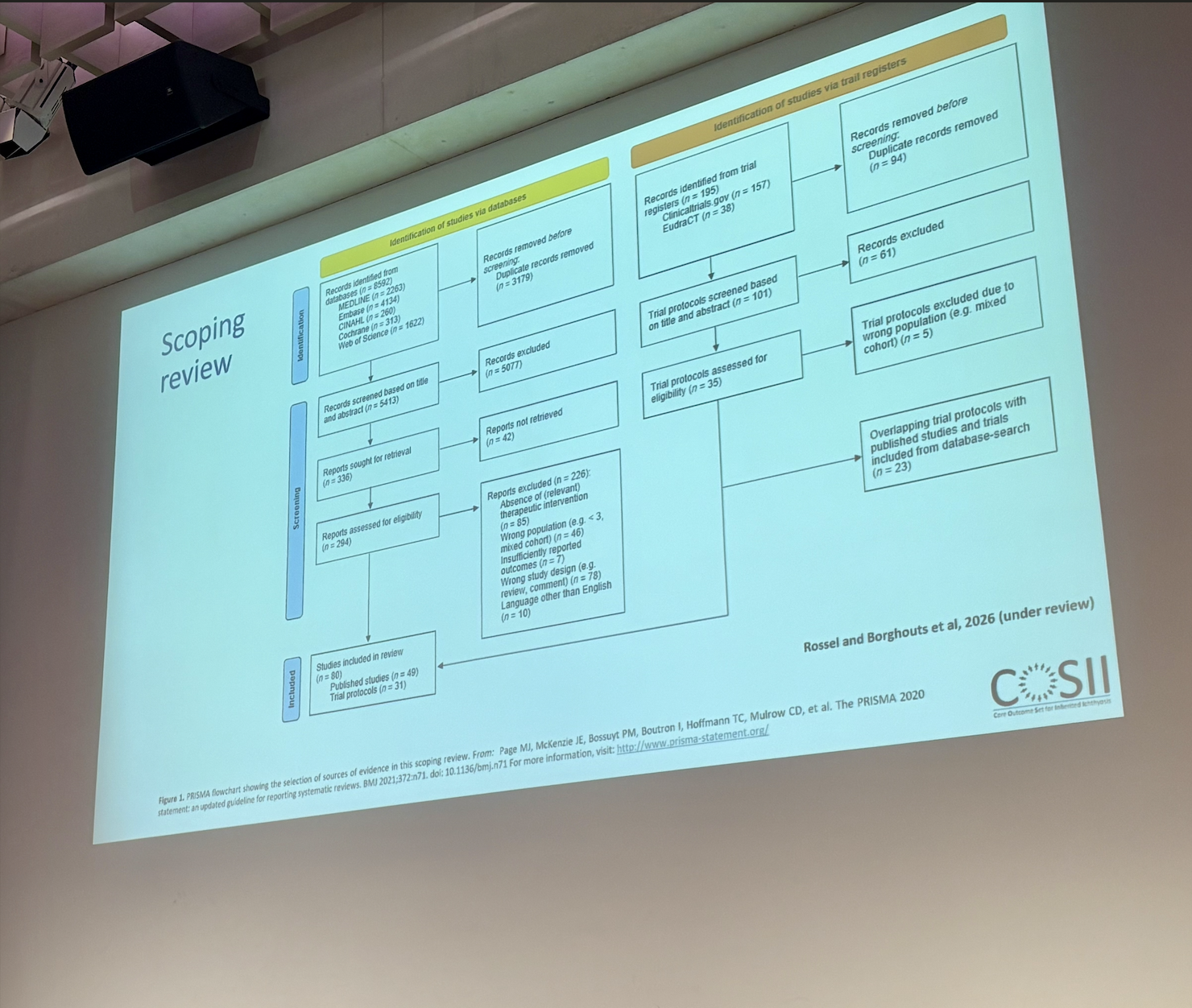
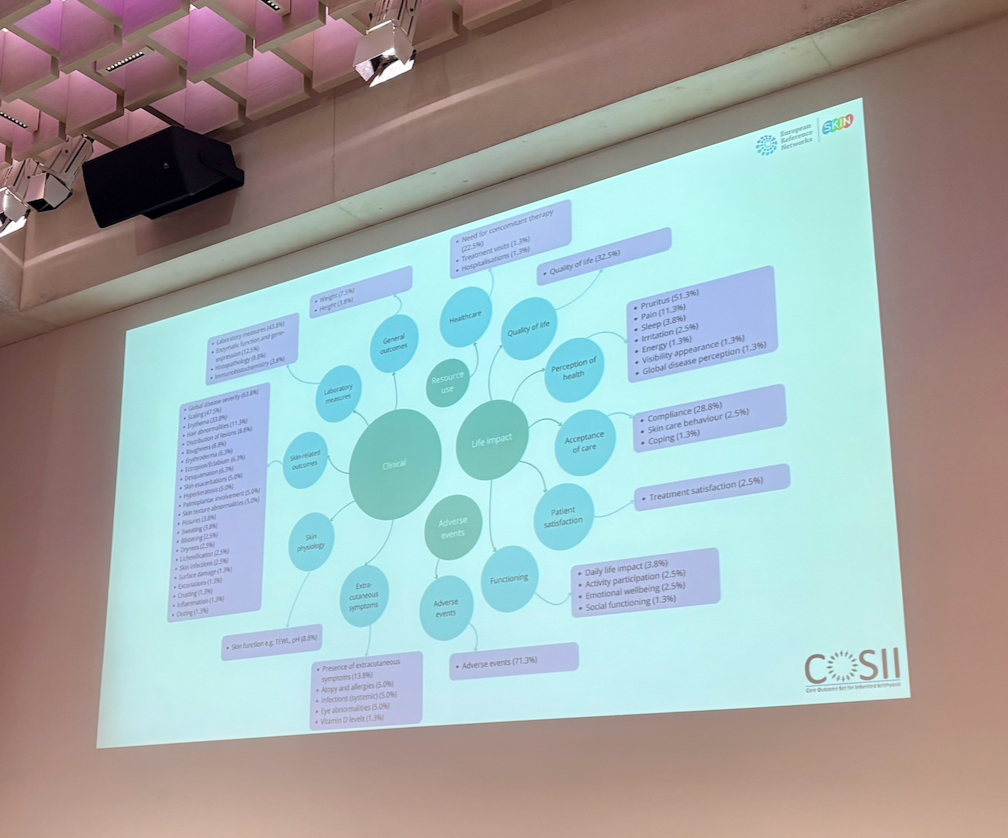
The final talk in Session 3 was delivered by Dr Antoni Gostynski (Netherlands) on the subject of measuring outcomes in EDDs. Dr Gostynski and his team are working on a collaboratively funded project, including a grant from EI Cure Project, to develop a new core outcome set for the inherited ichthyoses. Dr Gostynski explained the importance of having an appropriate core outcome set, in relation to ensuring new treatments can be measured using outcomes that are important to patients and clinicians, and then he went on to explain the process followed to develop the new outcome set. Dr Gostynski shared that his team had reviewed over 5000 studies for eligibility, and had been left with only 80 studies that met the inclusion criteria for the systematic review. The four key domains of “Clinical”, “Life Impact”, “Resource use” and, “Adverse events” were identified and further subdivided into 12 categories to be incorporated into the core outcome set.
Session 4) Gene Therapy and Gene Editing for EI
The final session of Day 1 was highly anticipated by everyone because each of the researchers delivering their talks have the potential to find a cure for EI in the long-term. Three out of the four research teams who presented their work are EI Cure Project Grant awardees, and it was such a pleasure to see so many different but brilliant approaches being explored simultaneously.
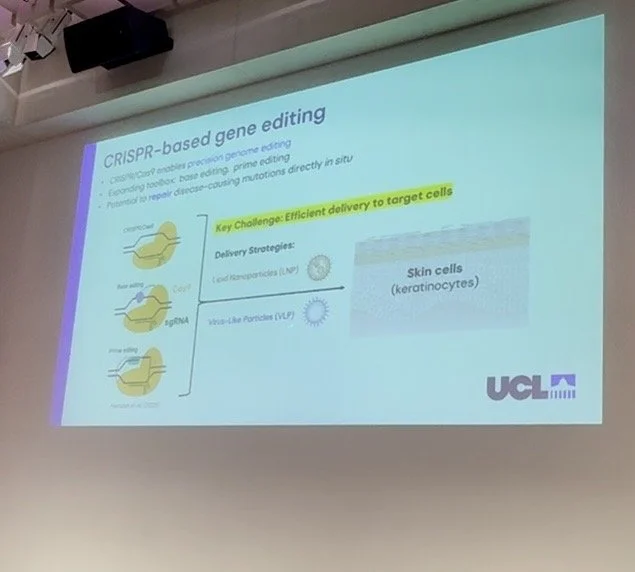
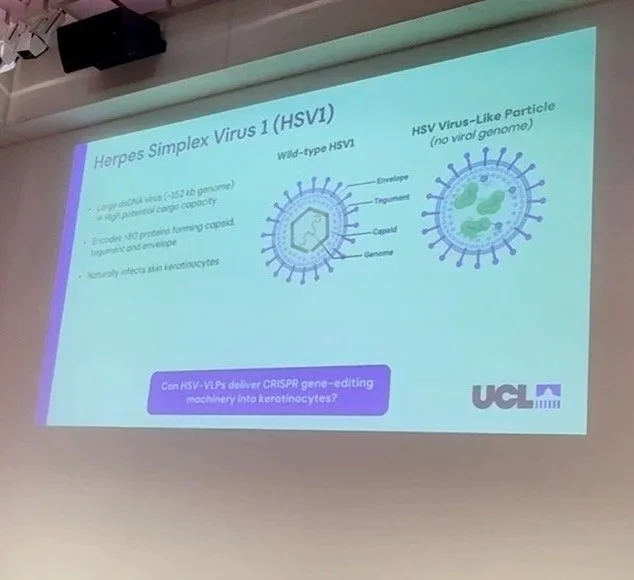
The first presentation of Session 4 came from Dr Amadeus Xu, a postdoctoral research fellow at University College London (United Kingdom). Dr Xu presented work from the first half of a 2-year research project with Professor Wei-Li Di and Professor Gill Elliot to explore the development of engineered virus-like particles to deliver gene-editing tools to skin stem cells. Dr Xu delivered an engaging talk to explain the process of extracting the disease-causing proteins from the Herpes-Simplex Virus, in order to replace them with gene-editing tools designed to correct the EI pathogenic variant. Dr Xu was happy to report that their project had met all their planned milestones and was on track for the next phase of the project, to explore if the modified virus can carry gene-editing tools to the skin stem cells in KRT1 and KRT10 EI models.
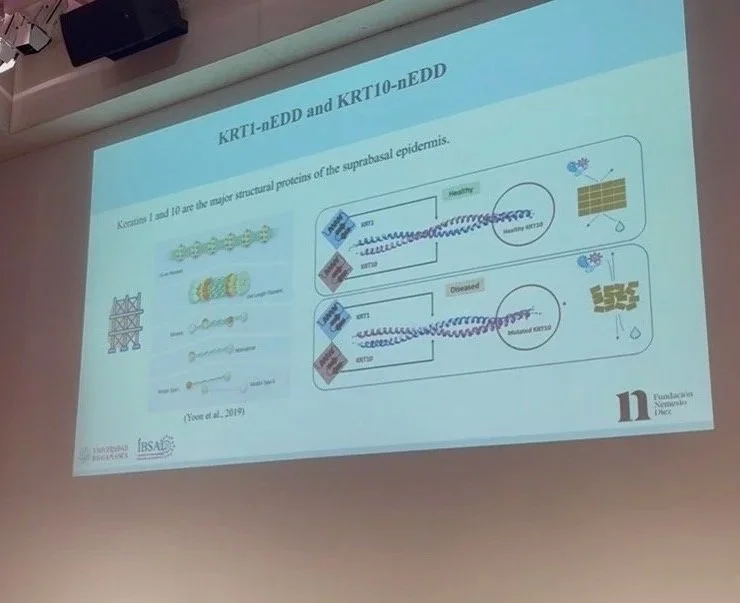
The second presentation was delivered by Maria Zubieta-Laseca, a PhD candidate from Spain. Under the supervision of Dr Irene Lara Sáez, of Instituto de Investigacion Biomedica de Salamanca, Maria presented her teams work using a non-viral approach to gene therapy using siRNA interference, otherwise known as ‘Gene silencing’. Maria explained the pros and cons of using gene-silencing in comparison to gene-editing, namely that the gene-silencing approach is less invasive, holds less risk, but would also require repeat dosing, whereas a gene-editing approach holds the promise of a cure with one treatment.
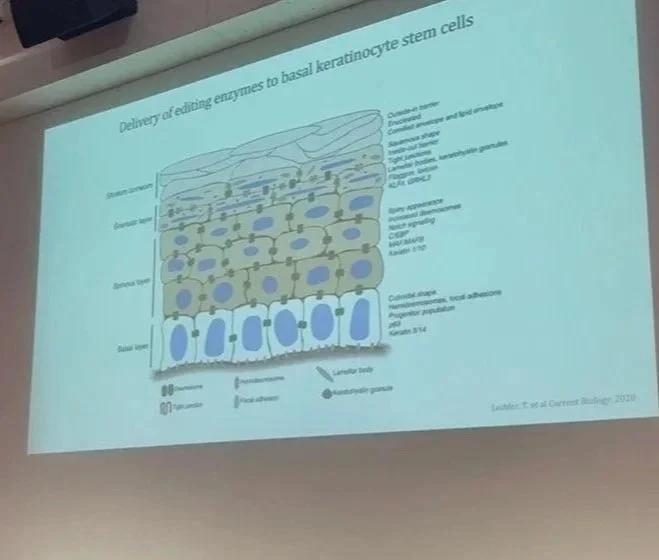
The third presentation was given by Dr Daniela Ortner-Tobider, an EI Cure Project Grant Awardee from Medical University of Innsbruck, Austria. Dr Ortner-Tobider presented work from the first year of a 3-year PhD project alongside the team’s PhD candidate Manuel Klump, and Principle Investigator Professor Matthias Schmüth. Dr Ortner-Tobider presented their work on “Advancing topical gene editing therapeutics for keratin-related skin disorders” including an explanation of the gene-editing tools chosen (lipid nanoparticles carrying a cytosine base editor) and the different methods they have used to try to transfect the skin barrier. At present, the team continue to try to find effective methods to ensure the gene-editing tools reach the optimal depth in the epidermis, at the level of the skin stem cells. Dr Ortner-Tobider’s talk provided a great deal of insight into the complex workings of gene-editing through intact skin. To date, topical delivery of gene-editing tools have only been successful through open skin wounds for patients affected with Dystrophic Epidermolysis Bullosa, so the work being conducted by Dr Ortner-Tobider and her team offers a real hope for many genetic skin disorders.
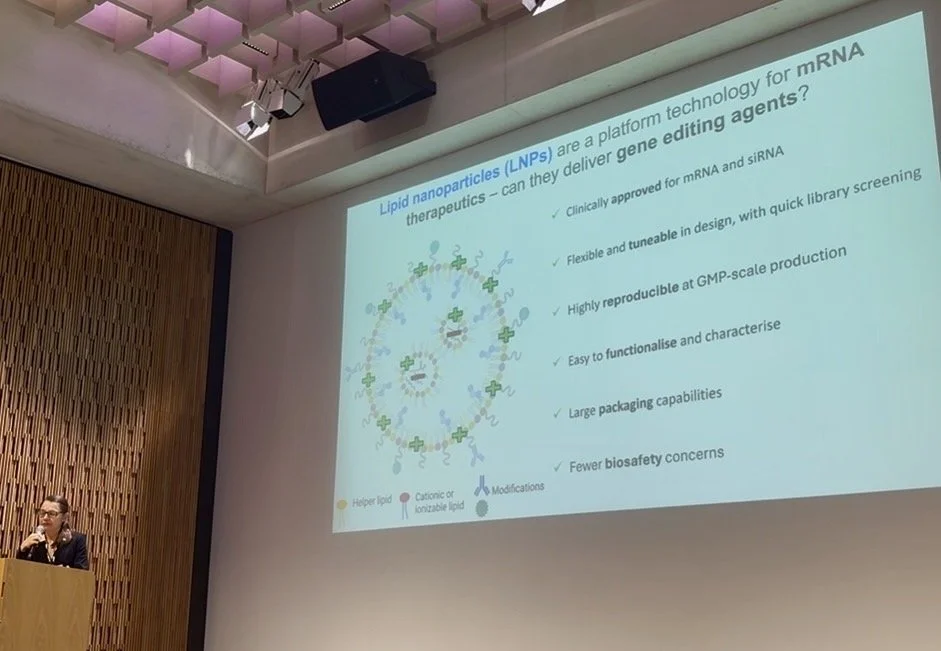
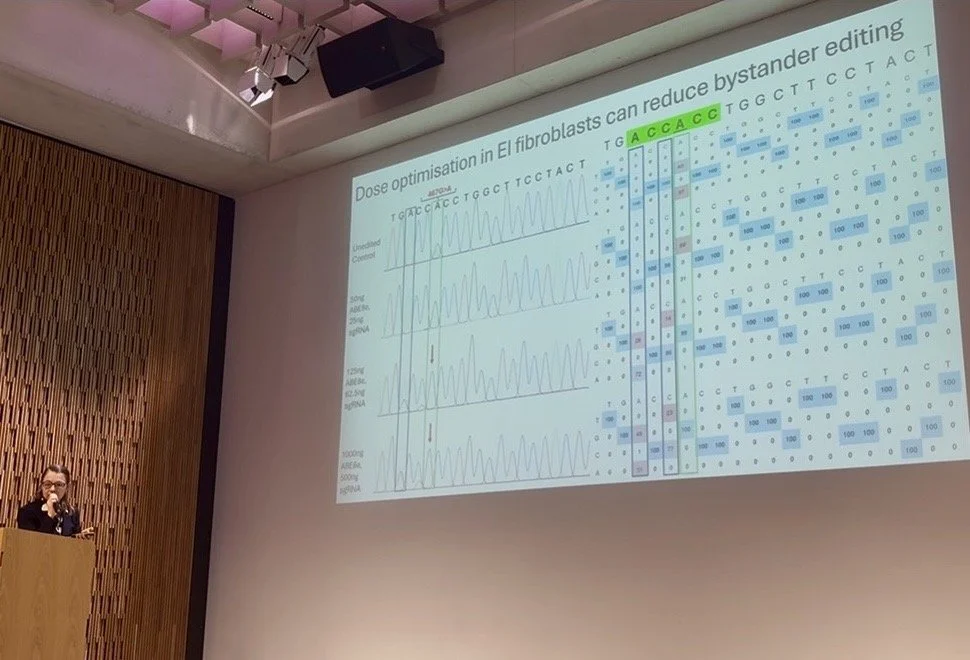
The final presentation of Session 4, and indeed the final talk of the Symposium, was delivered by the brilliant Dr Joanna Jacków-Malinowska, an EI Cure Project Grant Awardee, working in a research team at King’s College London with PhD candidate James Williamson and Co-Investigator Professor John McGrath. Dr Jacków provided a helpful introduction to her labs background in EB research before going on to explain how her team want to use their expertise to help those affected with Epidermolytic Ichthyosis as well. Dr Jacków explained that gene-editing tools have now developed beyond CRISPR-Cas9, and that base editors and prime editors should now be considered optimal tools for gene-editing. The 3 year PhD project using Lipid-nanoparticles with different types of gene-editing tools started for PhD candidate James Williamson in June 2025, so the research team are still in their first year. Dr Jacków explained that in their initial lab experiments they found that their chosen base editor located the mutation with accuracy, but with the initial dose used, the base editor also caused an unwanted ‘Bystander’ edit. By re-optimising the dose, Dr Jacków reported that the magnitude of the ‘Bystander’ edit was reduced. The project is still in the early stages, but EI Cure Project will continue to update the community when possible.
It was such an honour to bring all these brilliant minds together, and these new connections between early-career and experienced researchers will hopefully lead to new collaboration and even more ideas for further research in the future.
Day 1 of the EI Global Symposium was truly remarkable. For all groups represented—including researchers, scientists, clinical dermatologists, nurses, patient organisation representatives, and members of the EI community—it proved to be both enlightening and deeply moving. The discussions laid bare the realities of families living with EI while also revealing the first signs of genuine hope for the future.
Day 2 - Steering Committee Meetings
A total of 40 experts from Day 1 remained with us for a series of smaller group sessions designed to gain expert consensus on how to manage infections in EI, how to care for neonates and infants with EI, in addition to separate care guidelines for children, adolescents, and adults with EI. A total of four 90-minute sessions were led by four different group leaders, and directed overall by EI Cure Project Founder and Head of Research, Helen Lill.
For each group session, the group of 10 participants was altered to ensure a good mix of skills, and to encourage new and different perspectives to be brought to each group discussion. For each session, every group was asked to work through a series of statements taken from published evidence or directly from EI community practice. Experts were asked to decide whether to include, edit, or reject each statement, and had to decide on the level of evidence and grade of recommendation to support each statement using the SIGN Grading System (As used in the recently published “Management of congenital ichthyosis: European guidelines of care”).
Day 2 sessions were incredibly productive, and the group made good progress towards our goals of publishing consensus care guidelines in order to better support both patients and healthcare professionals in how to care for EI on a daily basis.
Formal Feedback for the Event
At EI Cure Project, this is the very first time that we have hosted such a big event, and as such we were keen to gain a better understanding of how our delegates really felt about the event. Delegates were invited to anonymously share their feedback on every detail of the event, from the food, to the venue, to the length of breaks compared to the timing of all the talks and group sessions, down to the speakers and the quality of their talks.
The comments and feedback about the event were wonderful to read, and we are so grateful to everyone who took the time to consider and write helpful and kind comments for the open questions. It was so wonderful to see that our experience of the event matched that of our friends and delegates.
Some comments from our delegates:
“I learned more than I could possibly ever write…”
— EI Community Member
“I have learned, and will change many things in my practice to benefit my patients”
— Clinical Dermatologist
“It was heart-breaking to learn about the everyday struggles — It makes us even more determined to help”
— Scientist / Researcher
“I was delighted to learn there are so many research projects happening for EI”
— EI Community Member
Some helpful feedback that we will take on board for the next symposium includes: 1) On Day 1, asking for adult volunteers to present their lived experience of EI; 2) On Day 2, having a parallel session for researchers and scientists to connect and exchange ideas; 3) On Day 2, inviting a guest panel or impartial mediator to help guide discussions on future directions for research.
“Thank you all for joining us at this future-defining event!”
— Helen Lill
(EI Cure Project Founder and Head of Research)